On Thursday evening, June 11, 2015, I was happily packing for our trip to Chincoteague to celebrate our 5th wedding anniversary. We were looking forward to walking on the beach holding hands, celebrating our anniversary at one of the local restaurants and strolling down Main Street in the evening enjoying an ice cream cone.
While I was talking to a friend on the phone that evening, my husband’s call beeped through. He usually called to tell me he was on his way home. I answered, “Hi honey!”
He said, “I’ve been in a motorcycle accident. I think I broke my back.”
That evening our lives changed forever.
We were to enter a world of hospitals and rehabs, paraplegics and wheelchairs.
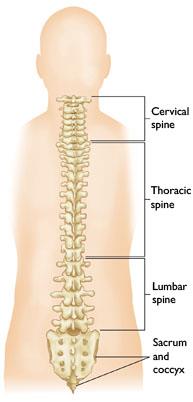
After X-rays, the doctor confirmed that Arthur’s back was broken at the T-11. The spine is made up of three parts – cervical, thoracic and lumbar. Arthur was fortunate; his injury was low on his back. Though he has no function or feeling below his bellybutton, he has full function above the break. It could have been worse. He could have died or been a quadriplegic.
In situations like this, you count your blessings. So many things are wrong that you grasp onto whatever light you can see.
On June 11, 2015, Arthur’s journey as a paraplegic began along with my journey as a caregiver.
When you have an accident such as this, there are the knowns – his spine was severed, he needed about six months of rehab – and the unknowns. It’s the unknowns that are the most challenging.
During Arthur’s time in rehab, he suffered pulmonary embolisms behind his lungs. Pulmonary embolisms are formed when a blood clot in the leg travels to the lungs. It would have killed him had he not gotten to the hospital on time.
He spent several days in the hospital recovering from the pulmonary embolisms before being released to a step-down rehab with a gentler schedule of OT/PT – about 1 ½ hours a day. We know now that he should have been released to a step-down when he was released from the hospital the first time. We were relying on the social worker to guide us. We didn’t understand the process or know the right questions to ask.
Arthur needed to learn how to live life in a wheelchair. Physical Therapy worked with him doing exercises to build up his upper body and his core strength to transfer himself from his wheelchair to the bed, to the shower, to the bathroom. While building up his strength, he used a sliding board. One end goes under the bottom of the person and the other end rests on wherever the person is transferring to – a car, a bed. Then the person slides across the board. Arthur used this until he had enough upper body strength to transfer on his own.
Occupational Therapy teaches the practical side of living – how to get in and out of a car, how to get around in a kitchen. Rehabs usually have a kitchenette set up and a vehicle available to learn these basic skills. OT also teaches how to transfer to the potty and how to take a shower.
Think of all the things you do daily. Now imagine doing them without legs.
After 13 months in and out of hospitals and rehabs, Arthur and I moved into a condo together.
There’s a phenomenon called “Institutionalized Thinking.” After being in a hospital setting for an extended period of time, the patient becomes dependent on others to do everything for him or her as they gradually become less able to think and act independently. Meals are prepared and delivered to the patient. If the patient wants to get out of bed, he/she asks an aide for help. If the patient needs water, he/she buzzes the nurse. After a year of this, Arthur was used to being waited on.
In the beginning, Arthur expected me to do many things for him, even get him a glass of water to which I kindly but firmly I replied, “Your wheels work. Get it yourself.”
That was the beginning of his journey back to independence and our journey to find a new normal.
At first, Arthur was afraid of everything. He was afraid to cook because he couldn’t see the pot. If hot water splashed and injured his legs, he wouldn’t feel it. He was afraid to take a shower or transfer to the commode without help because he might fall.
When you’re a paraplegic, falling is fairly common. A few weeks after we moved in together, Arthur was taking two of our grandkids for a walk. I was to follow in a few minutes when I heard my name being called, “ANGELA. ANGELA!” I looked out our third floor balcony and Arthur was lying on the ground in his chair, on his back. It’s like a turtle being upside down on their shell, with no way to flip them-selves over. I am too small to lift him myself. Fortunately, a neighbor came and lifted Arthur up. Falling is unnerving and jarring to the system and he often hits his head.
Paraplegics and those confined to a wheelchair have to watch their weight, since they have to be able to lift their own body weight to transfer. Arthur never had to watch his weight so this was new to him. He can no longer eat whatever he wants because he isn’t active enough to burn off calories.
Sometimes, people can be insensitive, parking in a handicap spot without a handicap tag. Once, in Cape May while eating in a restaurant, a woman came up to our table and yelled at me for calling the cops. She was illegally parked and I got yelled at. Not enough handicapped spaces and abuse of those spaces are big problems in the handicapped world.

Because Arthur has a van with a ramp, he needs to park in a handicapped spot with the white lines next to it. If one of those isn’t available, he will park diagonally over two spots and we put out a neon orange cone to discourage people from parking next to him. Once, coming out of a meeting, someone had parked in the striped portion next to the van. We had forgotten to put out the cone! Arthur couldn’t put the ramp down to get in the van. We waited a half hour or more for the owner to come out. She didn’t think she had done anything wrong!
Paraplegics have several on-going issues including bedsores. It’s important to avoid prolonged pressure on any part of the body. I regularly check Arthur’s back and feet, the most common areas. Wheelchair users are particularly susceptible if they stay in their wheelchair all day.
Another ongoing issue for paraplegics is Urinary Tract Infections. Since they cannot express urine naturally, they often self-cathe on a schedule to express the urine. Because a foreign object is being put into their body at regular intervals – in Arthur’s case every two or so hours – UTI’s are not uncommon. Arthur has a UTI about every six weeks. After several rounds of antibiotics, the body becomes immune to them and the doctor is challenged with finding a stronger drug.
When Arthur was released to our new home, I wanted to give him two things – his dignity and his independence. Loss of dignity happens to almost all quads and paras hospitalized for an extended period of time. Nurses, doctors, aids are coming in and out all day long, examining you, bathing you, changing you. Arthur needed to relearn what it meant to have privacy – for him and for me.
To get to and from from doctors’ appointments and rehabs, Arthur took a Metro Access bus. It’s a blessing that it’s available, but it’s an imperfect system. He would occasionally be left waiting an hour or more for pickup; the trip from home to DC could take 1.5 hours to 3 hours one way and he was often late for his appointments.
I encouraged him to get his license again. And he was scared. He learned he had to take a driving class which cost about $800 and were available only in a few places. After the class, he had to have a physical and get approved by a doctor. Then he finally took his driving test and passed the first time! We now own a lime green van which he drives using a knob on the steering wheel and hand brakes.
The daily life of a para is exhausting. Most things take much longer to do than before. A 5 minute shower takes 45 minutes. Getting dress is also long process. To put pants on, Arthur has to roll back and forth in bed, inching the pants over his bottom until he’s covered. To put shoes and socks on, he has a grabber that loops over his foot so he can pull his leg up and rest it on his opposite leg.
Many paras have ongoing pain. The pain could be from a nerve misfiring or a bone fragment in the organs. My husband experiences sharp pains in his abdomen that double him over. They have been un-diagnosed and keep him up at night, so he wakes up exhausted in the morning.
Once Arthur is in bed for the evening, he doesn’t get out again. Because of this, he keeps a container next to his bed with TV remotes, water bottles, nuts and other things he needs, since he can’t just easily hop out of bed to get a snack or something to drink.
We have a tempurpedic mattress that raises and lowers like a hospital bed, making it easier for him to transfer out of bed. The mattress also helps to avoid bedsores.

Four and a half years post accident, we have managed a new normal. We go to the movies, the theater and restaurants. Each day has its challenges, but we face them together and find joy in the little things – doing our morning meditation together, enjoying a cup of tea in the afternoon and holding hands watching TV together in the evening.
Please ask questions or share ways that you have found to have a new normal in your relationship. You can find me at https://www.facebook.com/groups/312477319482247
Angela DiCicco
The Italian Grandmama
Theitaliangrandmama.com
theitaliangrandmama@gmail.com

we have a freind 30 yrs of age and his fiance traveling from Australia. He wants to drive in Italy . How does he get the attachments for driving for the steering wheel , and do you think he will need to take a test etc.
Any information is appreciated. He is very independent
LikeLike
In the states, my husband needed to retake the driving test. He had the attachments professionally installed, however, I think they can be ordered online.
LikeLike