My husband Arthur is a paraplegic. On Tuesday, February 25, he had a follow-up appointment with the doctor who did his carpal tunnel surgery on Friday, February 14. Both hands were wrapped and he could not put any pressure on them. After the surgery, he couldn’t wheel his chair or take care of his bathroom needs so he required 24 hour care. It’s the reason he is in rehab.
We were surprised that he could use his fingers after the surgery. He had been worried that he wouldn’t be able to use his cell phone, his contact to the outer world, his connection to me.
His stitches were removed a week ago Monday. They are healing nicely, the stitches so fine that he’ll barely have a scar. Now he can put some pressure on his hands, up to the point where he feels pain.
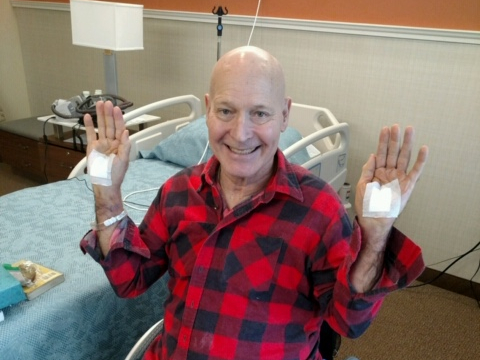
He asked me to take him to his follow-up appointment for the surgery as he is not yet driving. I agreed to take him in his van. His neon lime green van. I call it the Lean Green Arthur Machine. It’s a handicap accessible van fitted for Arthur. It has a knob attached to the steering wheel for his right hand to steer. I remove it so I can drive without it being in the way. It has hand controls on the left for the brake and gas. The brake and gas pedals have a safety plate in front of them to keep Arthur’s feet from accidentally sliding into them. I remove the two pins on the plate and lift it up and out so I can drive.
The van is large by my standards. The driver’s seat sits too far back for my little frame. Arthur is taller than me with longer arms. The seat is adjustable using motorized knobs on the side to move it up and back, making it easier for Arthur to transfer from his wheelchair into the driver’s seat. Adjusted as far up as it will go, it’s still not close enough for me to comfortably reach the pedals. I put a pillow behind me; it helps. I remember when I was 17 and learning to drive, my dad gave me a pillow to sit on.
My dad taught me a trick many years ago. He said when I drive a vehicle that I am not familiar with, tap the brake and the gas pedals a few times, back and forth with my right foot, getting comfortable with the feel of them, the distance between them, the shape and size of them. It is such good advice that I continue to use it today.
I adjust the side mirrors until I am comfortable seeing out of them. I turn to adjust the rear view mirror. One of the items required for Arthur’s driving test was a larger mirror. This one is about twice as long and high. It fits over the other mirror and takes a few moments for me to get used to it.
Arthur asked me to pick him up at the rehabilitation center approximately 11:45. His appointment is not until 1:10 but we allow for the extra time it takes to get him in and out of the van. I ask him to be ready and meet me out front so I don’t have to go into the rehab, sign the guest book and find him. When I arrive, Arthur was waiting for me in the vestibule.
I open the sliding door on the van and lower the side ramp using a button on the dashboard. A nurse going into the rehab center offers to help push Arthur up the ramp. Arthur normally has a portable motor that he uses when he goes out. It adds about 15 pounds to the wheelchair, and it helps going uphill and up ramps. We removed it and I took it home when he went into surgery since he wouldn’t need it. I am grateful for the nurse’s help.
After Arthur is inside the van, we anchor his wheelchair to keep it from rolling about in the back. We attach his front wheel to a hook on the floor. We have an extension on the seat belt that allows it to wrap around his body in the chair.
After I close the sliding door and settle myself in, I drive off. Does he have directions? He often waits until we are driving to think about directions. This causes me consternation because I am direction-challenged. However, I am familiar with the area that the appointment is in, traffic was moving and we arrive with plenty of time to spare.
We are fortunate that a handicapped space was available. You wouldn’t believe how rude people are! I’ve been yelled at for calling the cops on someone who was parked in a handicapped spot without a tag.
We’ve learned to put out an orange cone in the striped lines next to the handicapped spot. It deters drivers from “bleeding” into the van accessible spot making it difficult for Arthur’s wheelchair and ramp to fit. Or worse, a car will park in the striped area making it impossible for the ramp to come down.
We’ve spoken to other paraplegics and accessible parking is a problem they regularly deal with. Sometimes they sit it out and wait for the owner of the illegally parked vehicle to come out.
Inside the medical office, Arthur’s doctor is pleased with how his hands are healing. Arthur is free to transfer himself to his wheelchair, to the commode, to his bed as he is comfortable and the facility will allow. Currently he is being transferred from bed to wheelchair via a Hoyer lift– a portable pulley that lifts him up off the bed and sets him down in his wheelchair. Picture a stork with a baby in a diaper hanging from his beak.

Arthur asked for a script to transfer to National Rehab in Washington DC. He really wants to be an inpatient. The staff is stellar at this rehab and they have a focus on spinal injury.
At his current sub-acute facility, Arthur receives 1.5 hours/day of combined Occupational Therapy and Physical Therapy. At NRH, an acute rehab facility, he would receive 3 hours/day of OT/PT. He has to build up the upper body strength he has lost over the past several weeks since his surgery.
It’s the social worker’s job to grease the wheels for the transfer to another facility. It takes several days, tons of paperwork, many phone calls and both Arthur and me staying on top of the process. As of today, Thursday, he has not been approved. Arthur has been pro-active in following up with the social worker to make sure the paperwork has been sent over to NRH.
In January, Arthur started a new Medicare plan with Johns Hopkins. In this plan, NRH is an out-of-network facility. He was told that if he wants to transfer to NRH, he needs pre-approval. Today, Arthur is told that he will have to pay out-of-network fees. He makes yet another call to Johns Hopkins and is told that the representative is wrong. There are no additional fees. The rep who is misinformed is also the rep that approves or declines the request to transfer to NRH. It takes up to 72 hours for a response. It’s only been 48 hours.
After 20 days in a facility, Medicare increases the deductible to $100/night. We found out yesterday that Arthur’s 20 days were up. Today, he is being charged $100. It’s imperative that we get him transferred out tomorrow. If we don’t, he’ll be here through the weekend and on the hook for $100/night. Transfers don’t happen on weekends.
So our plan is that tonight he will stay where he is. Tomorrow, Friday, if he doesn’t get approved to transfer to NRH as an in-patient, I will take him home, where he can either have home health care or be an out-patient at NRH.
We have found that we must facilitate the changes that we want. Arthur must make the calls; we must follow up with the social worker, not once or twice but again and again. He is just one of many patients. If he isn’t a squeaky wheel, his case does not rise to the top.
One way or the other, Arthur will be out of his current facility tomorrow.
Angela DiCicco
The Italian Grandmama
theitaliangrandmama@gmail.com
theitaliangrandmama.com
Become a follower! Click the link and receive blogposts directly to your email.
Join our community on Facebook: https://www.facebook.com/groups/312477319482247/
